pressure injuries



why is this a priority for us?
- Pressure injuries occur when items push against the skin for prolonged periods and damage the skin and tissue underneath
- These can progress to open wounds and lead to infection, scarring, and prolonged hospitalization
who’s at greatest risk?
- Patients who are very sick, and those who are not moving much
- Patients who are not well nourished
- Patients who have objects such as casts, braces, face masks, or even oxygen sensors which can create pressure on the skin
what are we doing to help reduce pressure injuries?
- Routine checking of skin by a dedicated group of nurses, especially around medical devices
- Rotating oxygen probes twice daily
- Using moisture barrier creams with diaper changes
- Making sure we use the right bed for each patient
- Assessing patients for those who are at high risk for development of pressure injuries
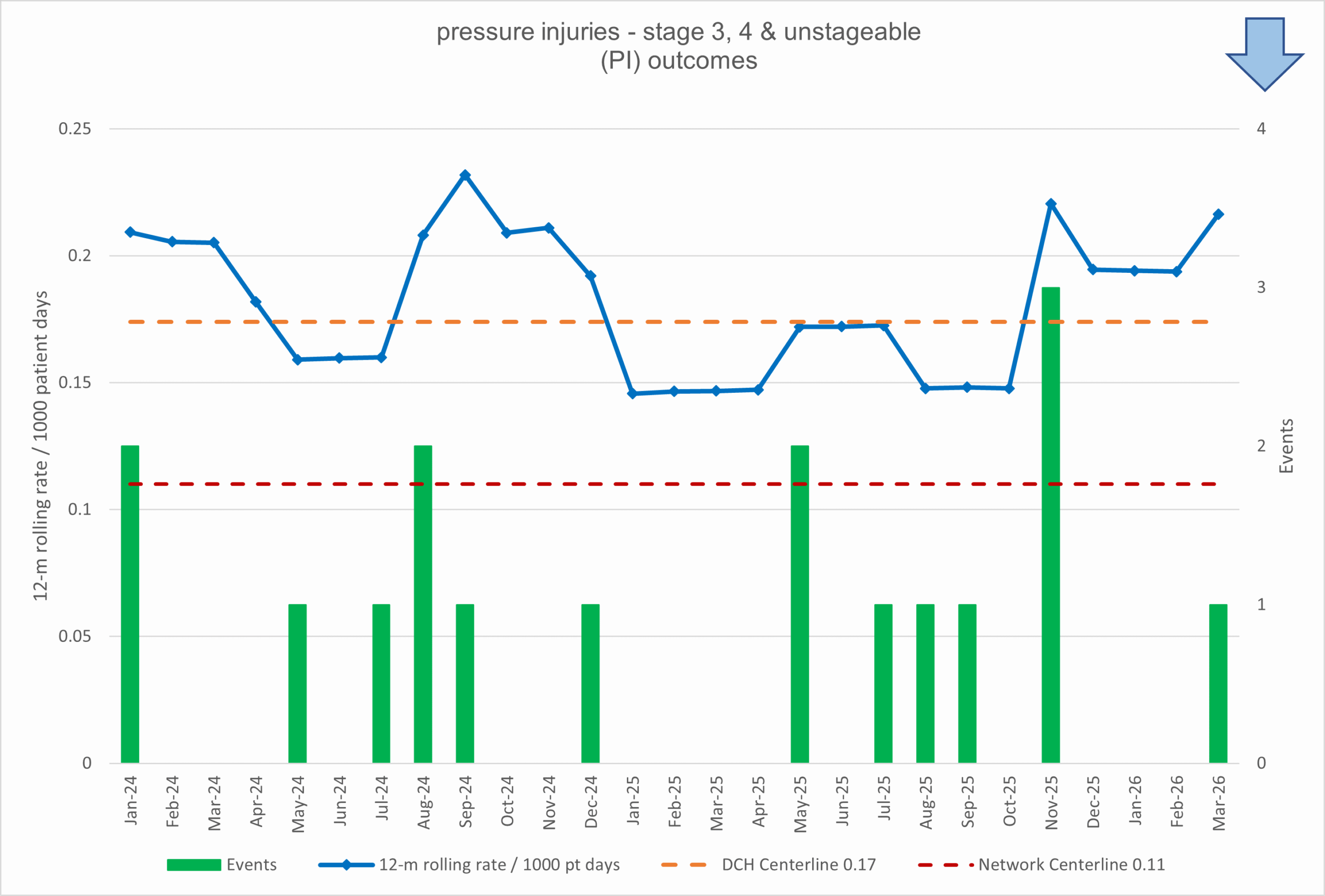
what do we measure?
We measure the number of pressure injury events per 1000 patient days.
related links
Visit the links below to learn more about how we measure quality and safety and overall patient experience.
explore care options
From the common to the complex, Dayton Children’s is here for you. Find a trusted provider who knows and understands kids, schedule an appointment online or find care now.
