tuberous sclerosis

about condition
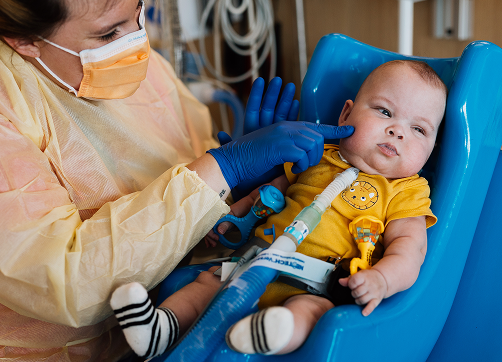
Dayton Children’s team of pediatric experts partner with the Tuberous Sclerosis (TS) Alliance to provide multidisciplinary care. TS is cared for in our TS Alliance-designated neurocutaneous clinic. In this clinic providers from neurology, neurosurgery, hematology-oncology, genetics and many other specialities work together to care for patients. Our patients are also able to see an ophthalmologist on the same day of their visit. Our multidisciplinary team provides state-of-the-art care for diagnosis of TSC as well as management of the different symptoms. We also help set up screening for the different signs of TS, as per the standard guidelines.
Our patients and their families are also supported by two social workers and a school nurse liaison. The school nurse liaison works with the child’s school system providing seizure education, identifying the academic needs of the child and aligning the medical and educational aspects of the child’s care.
Children’s Brain Tumor Tissue Consortium
Dayton Children’s Hospital has joined with Children’s Brain Tumor Tissue Consortium to launch a first-of-its-kind Pediatric Brain Tumor Atlas.
Dayton Children’s Hospital is working to further research efforts that may one day lead to better treatment and cures for TS.
Dayton Children’s neurosurgeon, Dr. Robert Lober, is one of a very few researchers practicing advanced research technology by operating a live tumor bank. “The tumors that we remove are grown in a dish so that one tumor can become 100 tumors that can be shared with reseachers all over the world.”


what is tuberous sclerosis?
Tuberous sclerosis, or tuberous sclerosis complex (TSC), is a rare genetic disease. It is caused by a gene mutation that causes tubers (benign tumors) to grow in different areas of the body, such as the brain, kidneys, heart and skin. Because of the many areas of the body that are affected by this disease, many patients can go misdiagnosed for several years. TSC affects 1 to 2 million people worldwide, and 25,000 – 40,000 within the United States. It is estimated that TSC affects 1 in 6,000 newborns.
what causes tuberous sclerosis complex?
TSC is caused by changes in either the TSC1 or the TSC2 gene. These genes help the body to control cell and tissue growth. The mutations in the gene lead to uncontrolled cell growth, and development of the tubers.


is tuberous sclerosis passed from a parent?
Because TSC is a genetic disease, it is possible that parents with the diease can pass the gene mutations to their children. If one parent has the gene mutation, then there is a 50% chance that their child will have it as well. There is no way to predict how mildly or severely the mutations might affect the child. If someone with TSC wants to have children, it is recommended they meet with a genetic counsellor to talk about their risk and options.
Often in patients diagnosed with TSC, there is no family history of the disease. With the TSC gene, there is a high rate of spontaneous mutation. This means that the gene changes on its own, and the change didn’t come from a parent.
what are the signs and symptoms of tuberous sclerosis?
Symptoms depend on what part of the body is affected by the tubers. The most common systems affected by tubers are the brain, heart, kidney, lungs, eyes and skin.
Brain
Tubers can grow in any part of the brain. Most people with TSC will have a seizure at some point in their life. One common form of seizures seen in infants with TSC is called infantile spasms. Some children may have refractory epilepsy. These can require advanced forms of treatment including special diets, placement of devices or a brain surgery by our highly-skilled neurosurgeons.
One-half to two thirds of patients with TSC have some form of developmental delays. These can range from mild learning disabilities to severe developmental delays. About one third of children with TSC show characteristics of autism. Many children also have behavioral issues such as:
- Attention deficit hyperactivity disorder (ADHD)
- Obsessive-compulsive disorder (OCD)
- Aggression
- Acting out
- Self-harm
Heart
Tubers that grow in the heart are called rhabdomyomas (rab-doh-mahy-oh–muhs). These are most commonly found in infants and young children. Many times they are seen in ultrasounds before the infant is born. If the tuber gets too large, or if there are several tubers, there is a risk of the tubers blocking blood flow to and from the heart. In most cases, these tubers are the largest at birth and shrink over time. Usually, they do not cause problems later in life.
Kidneys
Tubers in the kidneys are called angiomyolipomas (AN-jee-oh-MY-oh-lih-POH-muhs). They are found in 50% to 60% of patients with TSC, often between the ages of 15-30 years. These tubers are often found in both kidneys. They are made up of fatty tissue and muscle cells. Many times these tubers are small and do not cause serious problems. In some cases, they can grow large enough to affect kidney function and lead to bleeding, pain and kidney failure.
Lungs
Tubers may also grow in the lungs, especially in adults. When this happens, they can cause problems with breathing, shortness of breath and even a collapsed lung. Tubers are found in the lungs more often in women than in men.
Eyes
Tubers can be present in the eyes of some TSC patients. They show up as white patches on the retina of the eye. Most of the time, these do not cause vision loss or other medical problems. These can be helpful in diagnosing TSC.
Skin
About 70-80% of patients with TSC have skin lesions caused by the tubers. Skin lesions are lumps, bumps, sores or colored areas on the skin. Angiofibromas (AN-jee-oh-fy-BROH-muh) are small tubers that are commonly found under nails or on the scalp or face. Some patients might have patches of white skin, or areas of thickened skin. Other patients might have flat brown spots on their skin. These are known as café-au-lait spots. They might also have raised, discolored areas on the face, or reddish spots that look like acne. Most tubers on the skin do not cause any further medical problems, but can help in diagnosing TSC.
how will providers diagnose TSC?
Providers diagnose a patient with TSC based on their clinical findings. They often first start to look for TSC in infants and children with seizures, developmental delays, cardiac rhabdomyomas or skin lesions. Genetic testing helps to confirm the diagnosis of TSC. Tests or scans can also help diagnose TSC.
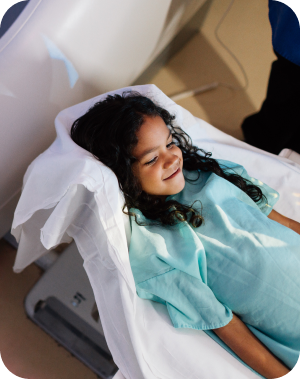

what tests are used to diagnose TSC?
- An MRI of the brain to look for tumors in the brain and renal system that often occur with TSC
- Echocardiogram (an ultrasound of the heart) to look for tumors on the heart
- Ultrasound to identify any kidney lesions
- Genetic testing to look for a TSC-related gene change
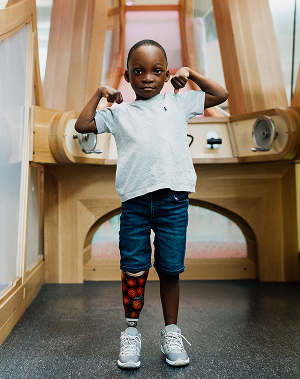
what doctor treats tuberous sclerosis?
Depending on your child’s signs and symptoms, he or she may be evaluated by several different specialists. They could include doctors trained to treat problems of the brain (neurologist), heart (cardiologist), eyes (ophthalmologist), skin (dermatologist), kidneys (nephrologist), and others.
what is the life expectancy of someone with tuberous sclerosis?
It can vary based on the patient, and depends on the severity of their disorder. Many patients with TSC live normally and have a normal life expectancy. All patients with TSC should follow up regularly with their providers to watch for any new symptoms or appearance of new tubers of lesions. Untreated and unnoticed tubers can lead to complications and even death.
related blogs
bad night’s sleep? how sleep impacts blood sugar in patients with diabetes
read morea breath of change: asthma awareness month and advancing health equity for children
read morehere when you need us
Whether you’re looking for the right provider, ready to make an appointment, or need care right now—we’re here to help you take the next step with confidence.



