news article
mapping the future of mental health
Dayton Children's expands services to help children in mental, behavioral crisis
“My child was in crisis. I didn’t know what to do or where to go. No place seemed to have a way to ensure he was safe and our family got the help we needed to stay whole. I felt lost, confused, overwhelmed, alone and utterly abandoned by a system that was supposed to help.”
the problem

That mother didn’t want to share her name, but her experience is universal. Last year, the Dayton Children’s emergency department evaluated nearly 1,000 children experiencing a behavioral health crisis. One in six families will need some sort of help for a mental and behavioral problem with a child. Many of them will not get the support they need because mental health has long been a gray area of care in our society, with frequent debates over classification and insurance issues that only add to the complexity for coordinated care.
In a survey of nearly 500 families and pediatricians in the area, Dayton Children’s 2017 Community Health Needs Assessment revealed mental health to be a top concern for the second survey in a row. While the hospital took several monumental steps after the previous assessment, it was clear more needed to be done.
“The services available to children in crisis are fragmented, duplicative and confusing for parents and professionals,” agrees Mary Beth Dewitt, PhD, psychology program manager. “With the closing last year of inpatient pediatric psychiatry services provided at Upper Valley Medical Center, our community has limited mental health services for children needing inpatient crisis stabilization.”
first steps
Dayton Children’s took a bold and innovative first step in 2012 to deal with this crisis and established the Mental Health Resource Connection program. This service serves as the gateway from the primary care physician to the appropriate mental health service in our community. What makes it so unique is the speed at which this connection happens and the personal connection that ensures each child gets to the right person at the right organization.
Here’s how it works: pediatricians and family medicine doctors make a referral to a trained social worker at Dayton Children’s. Within one day, that social worker calls the family and does an assessment over the phone. The social worker learns the specific issues and concerns that the family is dealing with and then, with in-depth knowledge of the agencies in the Dayton area, is able to connect the family to not only the right organization, but even the right person inside that organization.
This groundbreaking service solves two of the biggest problems families encounter when facing a mental health issue – slow response and a confusing system of services. No family can wait weeks for help with a mental health issue to then discover they are in the wrong place and have to start over again. It can also help with two other common concerns, unrecognized symptoms and financial concerns. The social worker at the Mental Health Resource Connection serves as a guide or a navigator to the family to leverage all the skills of each agency for the best outcome for the child.
Another key component of the program is the follow-up. Counselors continue to contact the family after the first assessment to make sure they got connected to services, provide them alternatives if they didn’t, and share results with the primary care physician who gave the referral. This ensures a circle of connected care surrounds the child and family.

The proof is in the performance. This program has seen a 243 percent growth in the past five years, connecting more than 3,600 children to services last year alone. Almost half the time, the child had an appointment with a provider in less than two weeks, 80 percent of the time in less than a month. More than half the parents perceived the therapy to be better after their interaction with the Mental Health Resource Connection and almost a quarter of those kids never come back to the emergency department in crisis.
Dayton Children's presented the program and results at the 2017 Children’s Hospital Association conference in New Orleans as a model for other hospitals around the country to emulate.
“The Mental Health Resource Connection program is the best thing Dayton Children’s has ever done. Being able to hand over patients to capable and caring hands at Dayton Children’s is a time saver, and reassurance for our staff and families.” – community pediatrician
building momentum
The need continued to grow, so did our services. A careful evaluation of every step of the Mental Health Resource Connection found more ways to improve, including identifying gaps in community services and further participation in regional plans to improve services. Over the next three years, Dayton Children’s strengthened partnerships, added mental health staff and found new ways to help parents.
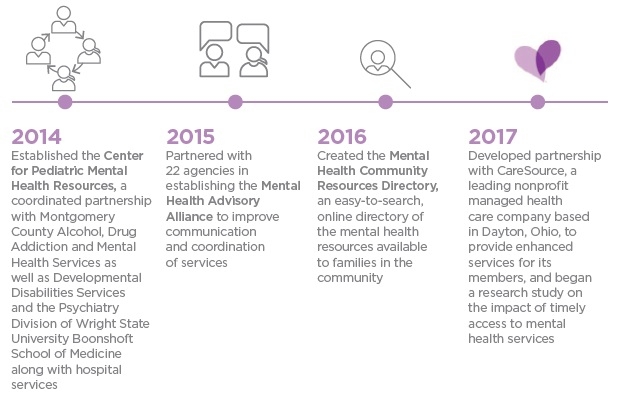
the future
When the results came back from the 2017 Community Health Needs Assessment, mental health ranked once again as a top priority so Dayton Children’s knew the work wasn’t done. Nine percent of children experienced two or more adverse childhood experiences (ACEs). These include abuse, neglect, violence or substance abuse in the home, divorce and incarceration of a family member. One-fifth of moms and one-tenth of dads rated their young child’s mental health as fair or poor.
That is why Dayton Children’s will develop a regional behavioral crisis center by March 2018. The centralized center will be next to the main campus emergency department to provide access to medical care, if required. Trained professionals will provide an assessment of children suffering a behavioral health crisis and connecting these children to the appropriate services. “While our emergency department staff do a wonderful job of caring for our medically ill or injured children, they are not fully equipped to assess a mental health crisis in a child,” says Mindy Schultz, manager of the crisis center. “This center will be staffed 24/7 to handle that need.”
By 2019, Dayton Children’s will establish a 12- to 20-bed inpatient mental health unit to provide needed stabilization care to children and then connect them to the appropriate follow up care.
“We know one agency can’t do it all and we have amazing resources in our community for mental health,” says Melissa Smith, manager of social work. ”So our job is to stabilize the crisis then to lead the community response to behavioral health needs through a collaborative partner network, with primary care physician support and comprehensive services provided by Dayton Children’s.”
“When a child’s mental health needs are unmet, it can have lifelong consequences,” says Deborah Feldman. “These can affect their school, home and personal lives immensely and it is imperative to address these issues as soon as possible and not wait until their later teenage years.”
“We are committed to making Dayton the safest place for kids to live, learn and grow,” says Feldman. “We see mental health as a crucial element to that mission and will do whatever we can to support the needs of our kids and their families.”

