pectus excavatum
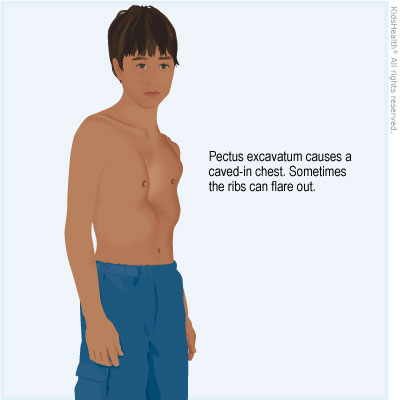 Pectus excavatum is a congenital deformity of the chest wall that causes several ribs and the breastbone (sternum) to grow in an inward direction.
Pectus excavatum is a congenital deformity of the chest wall that causes several ribs and the breastbone (sternum) to grow in an inward direction.
Usually, the ribs and sternum go outward at the front of the chest. With pectus excavatum, the sternum goes inward to form a depression in the chest. This gives the chest a concave (caved-in) appearance, which is why the condition is also called funnel chest or sunken chest. Sometimes, the lower ribs might flare out.
what causes pectus excavatum?
Doctors don't know exactly what causes pectus excavatum. In some cases, it runs in families.
Kids who have it often have other health conditions, such as:
- Marfan syndrome
- Poland syndrome
- Rickets
- Scoliosis
It's not clear how these disorders are related to pectus excavatum.
what are the signs and symptoms of pectus excavatum?
The main sign of pectus excavatum is a chest that looks sunken in. Even though kids who have pectus excavatum are born with it, it might not be noticed in the first few years of life. Many cases are found in the early teenage years.
Mild cases might be barely noticeable. But severe pectus excavatum can cause a deep hollow in the chest that can put pressure on the lungs and heart, causing:
- Problems tolerating exercise
- Limitations with some kinds of physical activities
- Tiredness
- Chest pain
- A rapid heartbeat or heart palpitations
- Frequent respiratory infections
- Coughing or wheezing
The condition typically gets worse as kids grow, and affects boys more often than girls. When a child is done growing, the pectus should not get any better or worse.
how is pectus excavatum diagnosed?
Healthcare providers diagnose pectus excavatum based on a physical exam and a child's medical history. If needed, they might also order tests such as:
- Computed tomography (CT) scan and/or a chest MRI to see the severity and degree of compression on the heart and lungs
- Echocardiogram to test heart function
- Pulmonary function tests to check lung volume
- Exercise stress testing to measure exercise tolerance
how is pectus excavatum treated?
Pectus excavatum can cause limitations to exercise and other physical activities or be completely harmless if it's not affecting how the lungs or heart work. Surgery often can correct the condition and treat any heart or lung issues. Physical therapy and exercises to strengthen muscles are also helpful.
what is Dayton Children's approach to treating pectus excavatum?
The surgery team at Dayton Children's has the experience, skill and modern equipment to treat patients with pectus excavatum.
- Vacuum bell: Designed for the non-surgical treatment of pectus excavatum, a vacuum bell is placed on the front of the chest and a pump is used to such the air out of the device. This creates suction, or a vacuum, that pulls the chest and breastbone forward. Over time, the chest wall and breastbone stay forward on their own and hold a new shape.
- Nuss procedure: To repair pectus excavatum, appropriate patients may undergo surgery that involves the Nuss procedure. The Nuss procedure involves placing a steel bar under the sternum to exert pressure to correct the chest deformity. The procedure itself is minimally invasive and requires two small incisions. The bar is removed two or three years later, once the deformity has corrected itself and becomes permanent. Ideally, this surgery is performed on patients ages 12-14. Any younger and the procedure would have to be repeated, and much older, the bones have hardened, making correction more difficult.
- Cryoablation: As a new approach to pain management, Dayton Children's offers cryoablation for pectus excavatum patients. The process uses extreme cold to freeze nerves and prevent pain. Using this approach, patients will be virtually pain-free following surgery without the use of opioids or other traditional pain medications and decreases their inpatient stay at the hospital.
Information provided by Dayton Children's specialists and KidsHealth.

