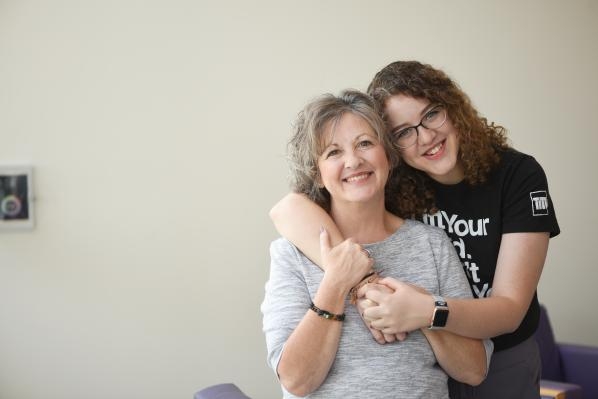Nov 12, 2019
A late night race for Elizabeth’s life
Elizabeth's Story
“My daughter is not going to make it.”
That was the horrifying thought racing through Susan Music’s mind as she frantically drove her 18-year-old daughter to the nearest emergency room late one night in April 2018.
Elizabeth was a senior in high school, already taking college courses and working a part time job. It wasn’t strange to anyone that she was often tired and stressed. Over the course of the year, she had lost 50 pounds, yet she was always hungry and excessively thirsty. She was cold all the time and would fall asleep in class nearly every day. Again, no one thought this seemed unusual, given her workload and activity level.
Elizabeth’s mental state was deteriorating. She was worried about these symptoms, afraid there was something seriously wrong, but she didn’t share her concerns with her parents. She didn’t want to scare them.
That day in April, Elizabeth was at work and became dizzy. She fell, hitting her back on a shelf. She was alone in the ice cream shop. She came to on the floor, picked herself up, and carried on until it was time to leave for tennis practice. When she got home, she fell asleep on the couch while her family ate dinner. Her body was in pain, but she thought she would sleep it off. “It’s wild to think that my body was literally slipping into a coma at that time,” she says.
Waves of pain and nausea awoke her later that evening. Her stomach was churning so she took an antacid and immediately vomited. She was struggling to breathe.
“My daughter changed colors,” says Susan. “My daughter was grey.” Finally, Susan knew there was something very, very wrong. She got Elizabeth into the car around 3 a.m. and raced to the closest emergency department, with no plan other than to find help.
Dayton Children’s South Campus was the first ER they came to, and Susan turned her car wildly into the parking lot. Elizabeth doesn’t remember anything after this frantic car ride, but every detail is etched in Susan’s memory.
“My daughter is not going to make it,” she yelled as she ran into the emergency room. “Somebody please get my daughter!”
ER staff came out of the woodwork, immediately jumping into action to get Elizabeth stabilized. For several agonizing minutes, the staff was unsure what was causing her symptoms. Then Andrea Self, clinical nurse, called for a glucose meter. Typical blood glucose is between 90 – 130 mg/dL. Elizabeth’s was over 1,000 mg/dL. Elizabeth was type 1 diabetic and was going through ketoacidosis.
The ER team needed to transport her to the main campus and into the PICU. Her glucose needed to come down very gradually through low doses of insulin. During the agonizing ambulance ride, Susan feared at one point that she had lost her daughter. But a determined paramedic wouldn’t give up on her and kept her conscious until they reached the hospital. “I’ve never seen such a team of people come together so quickly,” says Susan.
Elizabeth was in the PICU for five days. The first 48 hours were the hardest. That week, Elizabeth and her family had a crash course in type 1 diabetes and learned what their new normal was going to be. Now, she wears a glucose monitor at all times, which is connected to her and her mom’s cell phones so they both get alerts and can respond immediately when her blood sugar is too high or too low. “There’s not a night I don’t check on her,” says Susan. “We’ve learned not to wait and wonder – we just act.”
Elizabeth just finished her freshman year at Miami University, studying philosophy. She wants to go to law school and work in environmental justice. She has joined a student group of type 1 diabetics who not only support one another, but also do outreach projects like sending holiday cards to kids in the hospital.
“This is my life now, and no amount of denial or sadness is going to change that fact,” says Elizabeth. “It’s constant change and negotiation between what your mind wants and what your body is going to do. The biggest adjustment was learning how to deal with the way people look at you differently, even the people you love. It is a life-altering disease; there is just no getting around that.”
Susan says she feels “beyond blessed” to have had this experience at Dayton Children’s. She and Elizbeth has grown very close to her endocrinologist, Dr. Yelena Nicholson, who is available via text message day and night.
“Dayton Children’s will still be the place I could have died,” says Elizabeth. “But because of the fantastic staff and wonderful employees, I lived.”